Leg Ulcer Treatment
The below content has been medically reviewed and approved by Consultant Interventional Radiologist Dr. Mark Bratby (MBBS, MRCP, FRCR), Medical Director and Head of the Medical Advisory Committee at VeinCentre.
Last reviewed 1st August 2024.
Leg Ulcers
Leg ulcers develop when an area of skin breaks down to reveal the tissue underneath. Venous ulcers are the most common type of leg ulcer, with over 60% of leg ulcers being venous, according to NHS statistics. It is estimated that they affect around 1 in 500 people in the UK. They usually occur just above the ankle and can also carry with them pain and other symptoms such as:
- Itching
- Varicose eczema
- Discoloured or hardened skin
- Swollen ankles and heavy legs
- Active ulcers may also have discharge
We have 6 specialist ulcer centres offering this service:
Leg Ulcers Treatment
At Veincentre, we believe that living with ulcers is a thing of the past. We have over 20 years’ experience in treating venous leg ulcers via EVLA and foam sclerotherapy.
All our treatments are walk-in, walk-out and require no surgery. We find that these methods lead to quicker healing and longer-lasting results than traditional approaches. In our experience, leg ulcers tend to remain healed following this treatment pathway.

Step 1 – Consultation with your Dedicated Consultant
At Veincentre, your leg ulcer treatment journey starts with a simple ‘ABPI’ test to confirm whether the ulcer is venous (an issue with the veins), as we only treat venous ulcers at Veincentre. A colour duplex ultrasound scan is then performed, which confirms whether there is an underlying cause for the ulcers, i.e. varicose veins. The scan allows the consultant to look at the direction of blood flow inside the veins, as reverse blood flow indicates varicose veins. It is our experience that over 60% of ulcers are caused by venous issues however if we diagnose that the ulcer has another cause, our consultant will give you guidance on what to do next.
The results of your tests will be discussed there and then, along with a tailored treatment plan. The cost of this detailed appointment is £350.

Step 2 – Your Primary Treatment
The most common treatment for your ulcer is with Endovenous Laser Ablation (EVLA) to treat the underlying cause, and/or sclerotherapy. By fixing the underlying cause of your venous ulcers, this will allow the ulcer to start healing and remove the need for ongoing treatment in the NHS.
Once your treatment is complete and the veins have closed, the leg ulcer will heal relatively quickly as the underlying cause which led to the ulcer has been fixed. The wound will close up, the redness will fade, and any eczema will begin to clear up. In a small number of cases you may find that some pigmentation or scarring left from the ulcer, depending on the severity of it.

Step 3 – Follow Up Appointment
At your follow-up appointment, another scan is performed to check the underlying cause has been fixed. Often, the consultant will perform further sclerotherapy for any visible veins that are left to ensure you achieve your desired result.
Your follow-up appointment is recommended 6-8 weeks after the initial treatment.
We were delighted to see the results of the landmark UK-based EVRA randomised control trial published in the prestigious New England Journal of Medicine1 , which clearly supports our strategy. (EVRA is the acronym for the trial “Early Venous Reflux Ablation” .)
As the article itself states, this trial was the first to demonstrate that “early endovenous ablation of superficial venous reflux resulted in faster healing of venous leg ulcers and more time free from ulcers than deferred endovenous ablation”.
This followed an earlier study2 that had shown that traditional surgical correction of superficial venous reflux in addition to compression bandaging does not improve ulcer healing but reduces the recurrence of ulcers at four years and results in a greater proportion of ulcer-free time.
Although this earlier study had shown that surgical correction of venous insufficiency reduced recurrence, the fact that it also showed no improvement in ulcer healing held back the most effective treatment of venous leg ulcers by many years.
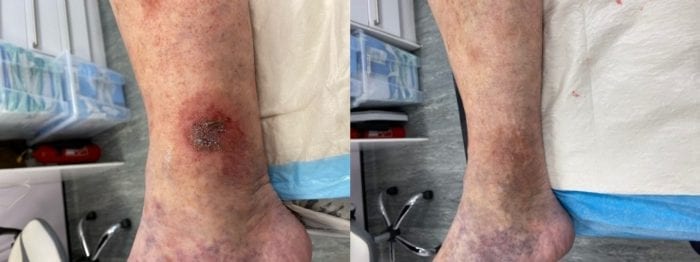
Leg Ulcer Treatment – Before & After
Venous leg ulcers appear as an open wound usually on the lower leg or ankle. The area around the wound will be red and there are likely to be skin changes such as venous eczema visible. If the ulcer is active, there may be discharge oozing from the wound, there may also be scabbed areas.
Following treatment for venous ulcers, the area will heal quite quickly. The wound will close up and the redness will fade, any eczema will begin to clear up.
 1
1

We are processing your answers – hold tight!
Complete Quick Online Assessment
Leg Ulcer Treatment Prices
We are committed to providing transparent pricing. All our prices are upfront and fixed, we have no ‘from’ prices. Please find these prices below.
1.
The VeinCentre Consultation
1-on-1 time with your vascular consultant
Comprehensive ultrasound scan
ABPI test
Personalised treatment plan
£350
2.
Treatment
EVLA addresses the root cause of varicose veins, while foam sclerotherapy targets visible veins, allowing the ulcer to start healing
NICE-endorsed as the treatment choice
Quick, walk-in, walk-out procedure with a 99% success rate
One Leg
£2,495
Both Legs
£3,350
3.
Follow Up
Includes another scan of your legs to check results
If needed, foam sclerotherapy to treat remaining visible veins
£250
Total
One Leg
£3,095
Both Legs
£3,950
Leg Ulcer Treatment Aftercare
We would advise you to continue with your simple dressing and wearing the compression stocking provided by VeinCentre for a week following EVLA and then to continue with dressings/bandaging provided from your GP surgery following this until the ulcer is fully healed.
Treatment Risks
With all medical treatments it’s important to weigh up the benefits versus the risks. With that in mind, we have provided you with a full outline of the known vein treatment risks.
References
1. A Randomized Trial of Early Endovenous Ablation in Venous Ulceration. May 31, 2018
N Engl J Med 2018; 378:2105-2114. DOI: 10.1056/NEJMoa1801214
(https://www.nejm.org/doi/full/10.1056/nejmoa1801214)
2. “Long term results of compression therapy alone versus compression plus surgery in chronic venous ulceration (ESCHAR): randomised controlled trial. BMJ. 2007 Jul 14;335(7610):83. doi: 10.1136/bmj.39216.542442.BE. Epub 2007 Jun 1.”
(https://www.bmj.com/content/335/7610/83)
